What causes white dry skin on feet depends almost entirely on WHERE on the foot it appears. Between the toes, it is almost always fungal. On the heels, it is usually thick dry callus with hyperkeratosis. On the sides, it is often eczema. The Body Map Diagnostic below lets you click your problem zone for the specific cause and fix.
What the Tool Below Will Tell You
The Body Map Diagnostic shows 6 foot zones: toes, between toes, ball of foot, arch, heel, and sides. Click whichever matches where your white dry skin appears. You will get the most likely cause for that specific location plus the targeted fix (antifungal vs urea cream vs ceramide cream vs trigger removal). Different zones, different problems, different fixes.
Body Map Diagnostic Tool
Click the foot zone where your white dry skin appears. Get the most likely cause and specific fix for that location.
Educational. Diabetic foot, non-healing wounds, or rapid color changes need a podiatrist evaluation today.
Why Location Matters More Than Anything

White dry skin can look identical from a distance regardless of cause, but the underlying drivers are different per zone:
- Between toes is a fungal environment 95% of the time (warm, dark, often damp).
- Heels are weight-bearing skin built thick that cracks under pressure + dryness.
- Sides of feet rub against shoes, making eczema and contact dermatitis common.
- Arch sweats less than other zones, so winter dryness shows up here first.
Treating all foot dryness the same is why so many people apply moisturizer to athlete’s foot (feeding the fungus) or apply antifungal to simple dry skin (irritating it).
Whatever the foot zone, skin barrier integrity depends on magnesium. Most adults run deficient, and the feet are one of the first places it shows (slow-healing cracks, dull skin, recurring dryness). Replacing nightly supports overnight skin repair where most healing happens.

Pure Encapsulations Magnesium Glycinate
400mg before bed. Supports the deep sleep where skin barrier repair happens, plus the ceramide synthesis that keeps foot skin from cracking.
Check Price on AmazonThe Universal Foot-Skin Reset (For Any Cause)
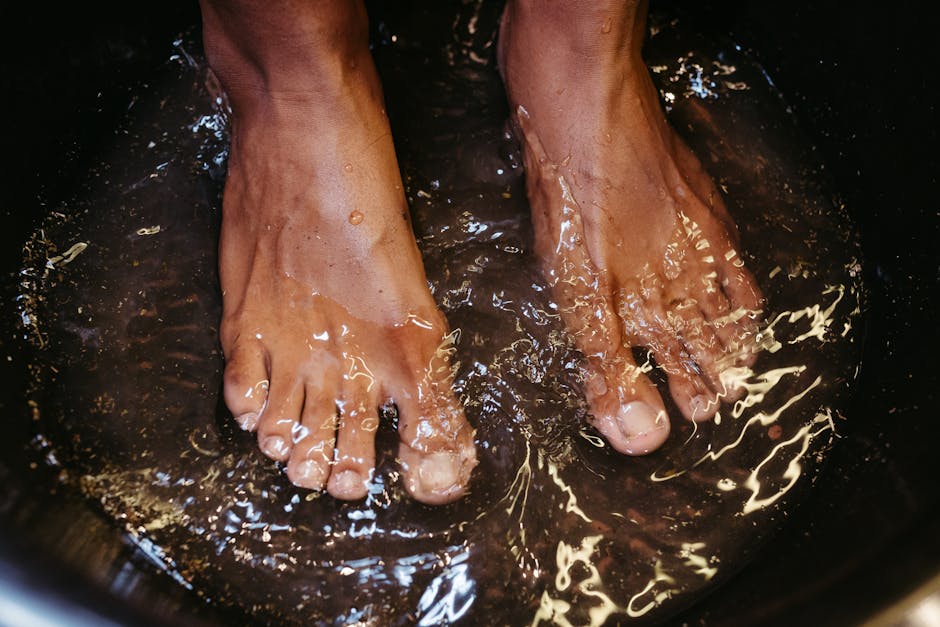
Regardless of location, the following protocol improves foot skin within 2-3 weeks:
- 15-minute foot soak 3-4 times per week. Warm (not hot) water, 1 cup epsom salt, 1 tablespoon olive or coconut oil. Magnesium absorbs through soles. Oil deposits onto skin.
- Pumice stone gently after soak. Only on heels and balls. NEVER between toes. 1-2 minutes per zone, not aggressive.
- Pat dry thoroughly. Especially between toes. Use a separate towel just for feet during fungal recovery.
- Moisturizer to damp skin. Urea-based (10-20%) for thick areas, ceramide for thin or sensitive areas. Avoid between toes if fungal.
- Cotton socks overnight after applying moisturizer. Occlusion massively boosts absorption.
- Hot showers OFF, lukewarm only. Hot water strips foot lipids.

Best Ingredients to Look For
- Urea 10-20% (general dry foot skin) or urea 25-40% (thick cracked heels). The strongest OTC humectant + exfoliant combo.
- Ceramides for skin barrier repair. CeraVe, La Roche-Posay, Skinceuticals lines.
- Glycerin as a humectant. In most quality foot creams.
- Coconut oil or shea butter for overnight occlusion under socks.
- Salicylic acid 6% for thick callus removal (use sparingly, 2x per week max).
Ingredients to Avoid
- Fragranced foot creams (often irritate)
- Alcohol-based products (further dry)
- Harsh sugar or salt scrubs (irritate dry skin)
- Strong essential oils undiluted (cause contact dermatitis)
If foot fungal issues keep coming back regardless of how aggressively you treat them topically, the question to ask next is whether systemic candida is feeding them. Activated charcoal as part of a gentle gut reset binds candida die-off toxins so they exit through the bowel.

Bulk Supplements Activated Coconut Charcoal
Take during candida-clearing protocols. Binds yeast die-off toxins. Two hours from food, supplements, and meds.
Check Price on AmazonWhen To See a Podiatrist or Dermatologist

- Deep cracks that bleed or do not heal in 2-3 weeks
- White dry patches that spread rapidly
- Pain when bearing weight
- Diabetes (any foot skin change in diabetics needs professional evaluation)
- Numbness or color changes along with dryness
- Fever or red streaking (signs of secondary infection)
- No improvement after 4 weeks of consistent treatment
Sock and Shoe Hygiene Matters Equally
- Cotton or wool socks ONLY during recovery (NOT synthetic).
- Change socks midday if feet sweat.
- Alternate shoes day to day so each pair fully dries 24 hours.
- Antifungal powder weekly in shoes if you’ve ever had athlete’s foot.
- Treat your bath mat too (wash hot weekly, fungal spores live there).
- Never share towels or pedicure tools.
Recurring Foot Skin Issues
When foot dryness or fungal issues keep coming back, the driver is often systemic. Find which toxic load pattern is yours in 90 seconds.
Open the ToolInternal Drivers Worth Investigating
- Hypothyroidism causes widespread dry skin including feet.
- Diabetes impairs healing and increases fungal risk dramatically.
- Iron deficiency (ferritin under 50) impairs skin barrier function.
- Zinc deficiency slows skin healing and barrier rebuild.
- Omega-3 deficiency shows up as scaly skin everywhere including feet.
- Chronic dehydration from caffeine, alcohol, or simply not drinking enough.
Bloodwork (TSH, ferritin, comprehensive metabolic panel, vitamin D) is worth pulling if foot dryness is part of broader skin or energy issues.
Frequently Asked Questions
What causes white dry skin on feet?
Depends on location. Between toes is almost always fungal. Heels and balls are usually hyperkeratosis with dryness. Sides are often eczema or shoe friction. Arch is typically simple xerosis. Click the body map zone above for the specific cause.
Is white skin on feet always fungal?
No. Between toes, almost always fungal. Other locations are more often dryness, eczema, psoriasis, or callus. Diagnosis depends on WHERE the white skin appears.
How do I tell if my dry feet are fungal?
Fungal: between toes, intense itch, sometimes yeasty smell, does NOT improve with moisturizer. Dry skin: heels and balls, mild itch, no smell, improves with moisturizer in 1-2 weeks.
What is the best treatment for white dry feet?
Depends on cause. Fungal: clotrimazole or terbinafine 2x daily 2 weeks past clearing. Dry skin: urea 10-20% cream + cotton socks overnight. Cracked heels: urea 40%. Eczema: fragrance-free cream + identify trigger.
Related Reading
- Athlete's Foot vs Dry Skin Diagnostic Tool — Differentiate fungal from dry skin overall
- Dry Skin Under Eyes Visual Type Finder Tool — When dryness shows on the face too
- Find Your Toxic Load Pattern — When skin issues persist across multiple body zones
Educational only. Diabetics with any foot skin change need professional evaluation. As an Amazon Associate I earn from qualifying purchases.





